Tinea Versicolor: Causes, Symptoms, & Treatment
What Is Tinea Versicolor?
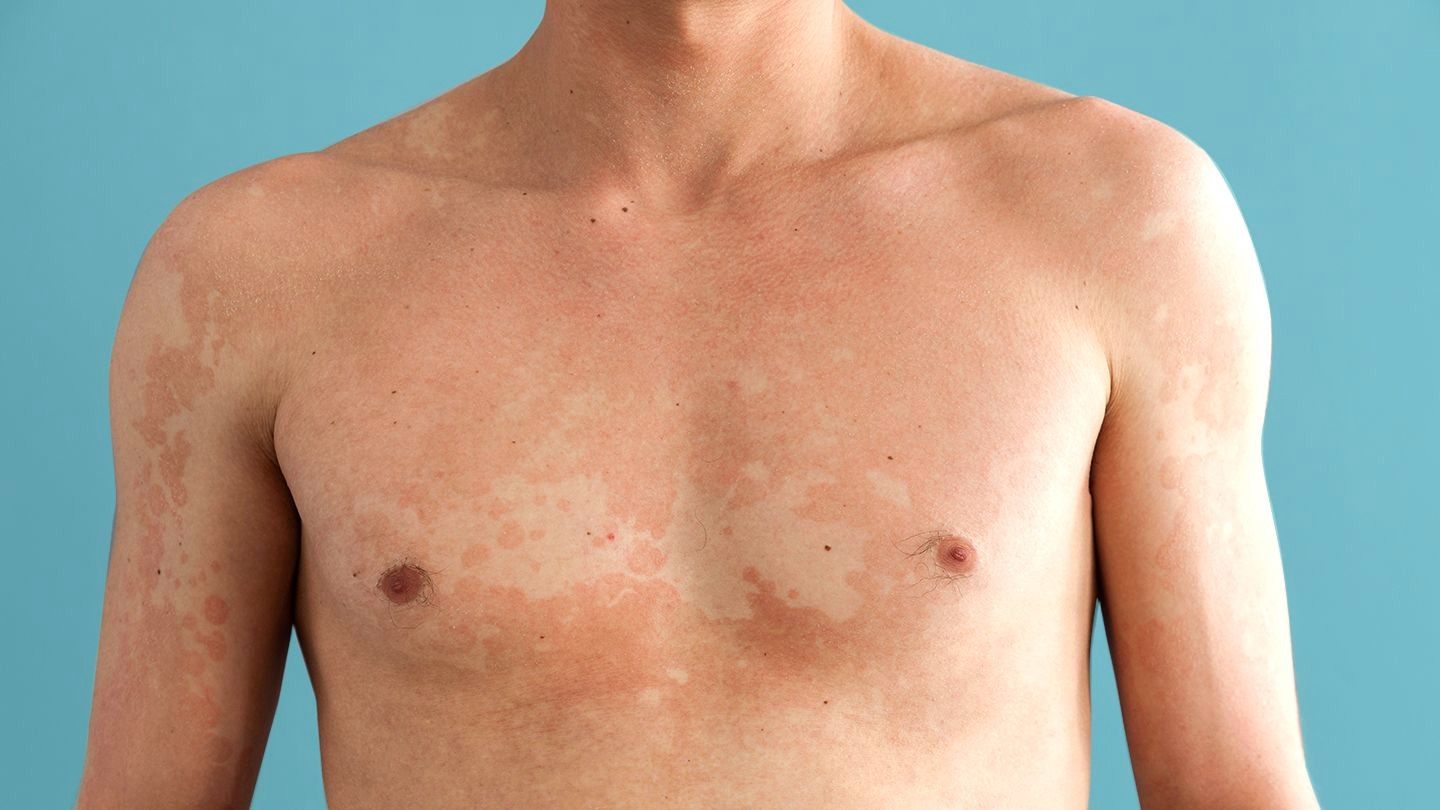
Tinea versicolor is a fungal infection that causes tiny patches of discoloured spots on the skin. It’s also known as pityriasis versicolor. It’s caused by a kind of yeast that naturally lives on the skin. When the yeast grows beyond control, the skin disease, which appears as a rash, is the consequence.
Signs and Symptoms of Tinea Versicolor
Acidic bleach from the growing yeast causes areas of skin to be a different colour than the skin around them. They can be small spots or patches. The symptoms and signs of infection are:
- Patches that appear red, pink, white or brown and may be darker or lighter than the skin around them.
- Spots that don’t tan the way the rest of your skin does.
- Spots that pop up more boldly when you do tan.
- Spots that can occur anywhere on your body but are commonly noticed on your chest, neck, back, and arms.
The spots may disappear during cold weather, but they can get worse during warm and humid weather.
Similar conditions
Some skin conditions have symptoms that look like tinea versicolor. These include:
- Vitiligo: It is a condition that makes you lose your skin colour
- Pityriasis rosea: It is a rash that can cause tiny spots that spread across your body in the shape of a tree
These conditions have features that clue your doctor into what you have, like the texture and rash pattern.
Tinea Versicolor Causes
The yeast responsible for tinea versicoloror, Malassezia, develops on normal healthy skin. However, these factors can cause an overgrowth that causes the infection:
- Oily skin
- Living in a hot climate
- Sweating a lot
- Hormonal changes
- A weak immune system
Since the yeast naturally grows on your skin, tinea versicolor isn’t transmissible. It can affect people of any skin colour. It is typically seen in teenagers as well as young people. For some people, it may cause emotional distress and feelings of self-consciousness.
Tinea Versicolor Treatment
How do dermatologists diagnose tinea versicolor?
A doctor can diagnose tinea versicolor based on how the rash looks like.
If they need more details, the following tests can help:
- Wood lamp (black light) examination: The doctor uses ultraviolet light, which may make the affected areas appear as a fluorescent coppery orange colour if it is the result of tinea versicolor.
- Microscopy using potassium hydroxide (KOH): The doctor will remove the cells from your skin, soak them in potassium hydroxide, and then analyse them under a microscope.
- Skin biopsy: The doctor will take an adipose tissue sample by scraping a small amount of skin and scales from the affected area for examination under a microscope. In the case of children, the doctor may remove skin cells by first firmly attaching transparent tape over the affected area before removing it. The sample can then be put directly onto a slide for examination with a microscope.
How do dermatologists treat tinea versicolor?
The treatment a dermatologist prescribes is based on a variety of factors. These include where the tinea versicolor appears on your body, how much of your skin is affected by tinea versicolor, how thick the spots have grown and the climate.
Treatment for tinea versicolor may include the following:
- Medicine applied to the skin: This is the most frequently used treatment. There are anti-fungal soaps, shampoos, creams, and lotions that can keep the yeast in control. They contain active ingredients such as selenium sulphide, ketoconazole or pyrithione zinc.
- Medicated cleansers: Tinea versicolor often returns, particularly if a person lives in a humid and warm place. Using a medicated cleanser at least once or twice a month, especially during hot and humid times, will stop the yeast from growing again.
- Anti-fungal medications: A dermatologist may prescribe these medications if tinea versicolor covers a significant area of the body, is thick or often reoccurs after it is treated. These medications are used for a limited time. During this period, your dermatologist will monitor you.
- Antifungal Soaps: There are several options available in the Indian market, but Ketoconazole-based soaps are considered the best antifungal soap in India for treating Tinea Versicolor.
Outcome
With treatment, the yeast is easy to kill. But, the skin can stay lighter (or darker) for a few weeks or even months. However, the skin will eventually return to its normal colour. To even out your skin’s tone, protect your skin from the sun and not tan.
Tinea versicolor can return. When the outdoor air is humid and hot, it is possible for the yeast to increase in size and become out of control. Some people who live in a tropical climate may need to apply a medicated cleanser year-round to prevent the yeast from over-growing. People who live in an area that becomes moist and warm each spring may see tinea versicolor come back every year.
Lifestyle Tips for Managing Tinea Versicolor
Episodes are very common since the yeast that causes the infection is a normal fungus that lives on your skin. You might use the medicated cleanser once a week for about 10 minutes for a few months to help prevent tinea versicolor from returning. It is possible to use these products if the infection keeps returning, especially for those who live in a humid and warm area.
If the condition is mild, it is possible to treat it yourself. There are anti-fungal products that you can purchase without a prescription. They include:
- Shampoo that contains selenium sulphide
- Anti-fungal cream or ointment that contains miconazole, clotrimazole or terbinafine.
When using these products, dermatologists suggest the following:
- Wash and dry the affected skin
- Apply a thin layer of the anti-fungal cream or ointment. Apply it at least once or twice a day for at least two weeks.
- If you are using a shampoo, leave it on your scalp for 5 to 10 minutes before cleaning it off.
- If you have oily skin, it’s best to use a dermatologist-recommended soap for oily skin to help manage the condition.
Some people require stronger medication which is why they consult a dermatologist. If you choose to treat yourself or consult a dermatologist, these guidelines will help you achieve better outcomes:
- Avoid using skin care products that are oily. Make sure you use oil-free products. The label may also read “non-comedogenic.”
- Wear loose clothes. Nothing should feel tight.
- Make sure your skin is protected from the sun. A tan makes tinea versicolor easier to spot.
- Avoid using a tanning bed or sun lamp. Again, a tan makes tinea versicolor more visible.
How can you protect your skin from the sun
To achieve the most effective results, it is essential to protect your skin from the sun. For this, apply sunscreen daily. Make sure that you apply sunscreen for at least 20 minutes before leaving. And apply it to all skin that will not be covered by clothes. Make sure you use a sunscreen that provides:
- UVA and UVB protection (label may read broad-spectrum)
- Sun Protection Factor (SPF) of 30 or more
- Non-greasy formula (label may say “oil-free” or “non-comedogenic”)
The Empowerment of Women’s Health: Nurturing Holistic Well-being
In today’s progressive era, women’s health has emerged as a pivotal topic, deserving special attention and care. The empowerment of women in all spheres of life is directly intertwined with their well-being, making it essential to prioritize and foster their physical, mental, and emotional health. Recognizing the unique challenges faced by women and embracing a holistic approach to their healthcare is key to ensuring a brighter and healthier future for all. In this article, we will explore various aspects of women’s health and highlight the importance of comprehensive care tailored to their specific needs.
Physical health forms the foundation of overall well-being, and women’s bodies undergo significant transformations throughout their lives. Regular medical check-ups, including reproductive health screenings and breast examinations, are vital for early detection and prevention of potential issues. Furthermore, adopting a healthy lifestyle through regular exercise, balanced nutrition, and adequate sleep is crucial for maintaining optimal physical health. Women should prioritize self-care and make informed choices about contraception, pregnancy planning, and sexual health to ensure their bodies are nurtured and protected.
Mental health is another critical facet of women’s well-being that deserves utmost attention. Women often bear the weight of multiple roles and responsibilities, and this can sometimes lead to stress, anxiety, or depression. Creating a supportive environment that encourages open dialogue and seeks to break the stigma surrounding mental health is paramount. Accessible mental health services, including therapy and counseling, should be readily available to help women navigate the complexities of their lives and build resilience. Empowering women to prioritize self-care and mental well-being will enable them to thrive and contribute fully to society.
Addressing women’s health also entails recognizing the unique challenges faced by different age groups. Adolescence marks the onset of several physical and emotional changes, making it vital to provide comprehensive sex education and support for young girls. Menstrual health education, access to sanitary products, and guidance on reproductive health are essential to ensure their smooth transition into womanhood. Similarly, during the reproductive years, comprehensive preconception, prenatal, and postnatal care is crucial to safeguard both the mother’s and child’s health. Supporting women through menopause, a phase that brings its own set of challenges, is equally important, ensuring women receive appropriate guidance and assistance to navigate this transformative period.
In addition to physical and mental well-being, it is imperative to acknowledge the social determinants that impact women’s health. Factors such as education, economic opportunities, and access to healthcare services significantly influence their overall quality of life. Promoting gender equality, bridging the wage gap, and providing equal opportunities for education and employment can positively impact women’s health outcomes. Additionally, ensuring access to affordable healthcare and eliminating barriers to care, such as transportation or child care, will empower women to seek the medical attention they need.
Women’s health cannot be discussed without considering the importance of preventive care. Regular screenings for cervical and breast cancer, vaccinations against HPV and other infectious diseases, and proactive measures to prevent osteoporosis and heart disease are essential components of preventive healthcare. Encouraging healthy habits, promoting self-examinations, and raising awareness about the early signs and symptoms of various health conditions can save lives and reduce the burden on healthcare systems.
In conclusion, the empowerment of women’s health goes beyond the boundaries of individual well-being. By prioritizing comprehensive care, including physical, mental, and social aspects, we can create a society that uplifts and supports women at every stage of their lives. Embracing a holistic approach to women’s health ensures that they are equipped to face challenges, pursue their dreams, and contribute meaningfully to society. It is our collective responsibility to advocate for and invest in the well-being of women, as their health is an indispensable asset for a prosperous and harmonious future.